Dr. Sean B. Rourke, MAP scientist, spoke to the CBC for a story about a Our Healthbox vending machine being introduced at the People of the Dawn Indigenous Friendship Centre in Stephenville, N.L. The machine, unveiled Wednesday, has naloxone and HIV self-testing kits, safe consumption supplies like clean needles, sexual health supplies, as well as menstrual and hygiene products, and traditional medicines kits.
Month: February 2026
Our Healthbox lands in Newfoundland: Free health supplies now within reach thanks to Staples Canada
Stephenville, Newfoundland – Feb. 25, 2026 – St. Michael’s Hospital’s MAP Centre for Urban Health Solutions and People of the Dawn Indigenous Friendship Centre (PDIFC) are thrilled to announce the launch of Newfoundland and Labrador’s first Our Healthbox, thanks to generous support from Staples Canada through their Even the Odds partnership.
Located at 35 Carolina Avenue in Stephenville, the People of the Dawn Healthbox will distribute free health and wellness supplies such as HIV self-test kits – including the OraQuick oral swab HIV self-test – Naloxone kits, harm reduction and drug screening kits, sexual health items, traditional medicines, snacks, nutritional drinks and period packs.
PDIFC is a non-profit organization that delivers culturally appropriate services to Indigenous people – regardless of status – in urban communities. The Centre provides services and supports to assist people with challenges related to employment, health, education, justice and housing.
“This project and its partnerships continue our commitment to meeting the health needs of our community in meaningful and innovative ways,” said Patrick Park-Tighe, executive director of People of the Dawn Indigenous Friendship Centre.
“We are very excited about this project launch as it lowers barriers to access for individuals while letting them choose how to engage with the resources and supports most essential to them. We look forward to introducing visitors and clients to this new and novel addition to our Centre.”
Developed by Dr. Sean B. Rourke, director of REACH Nexus at the MAP Centre for Urban Health Solutions, Our Healthbox units feature interactive touch screens integrated into commercially available vending machines, transforming them into accessible hubs of community wellbeing that give people what they need to take care of their health, when they need it.
These cutting-edge machines offer free, low-barrier access to HIV self-test kits – empowering individuals to know their status – harm reduction supplies as well as potentially life-saving Naloxone kits to reverse opioid overdoses. The machine also provides wellness products, including menstrual and hygiene supplies, and seasonal essentials such as hats and gloves, tailored to the unique needs of each community.
“Everyone in Canada has the right to healthcare and yet fa rtoo many people are being left behind,” said Dr. Rourke. “We’re excited tobring Our Healthbox to Newfoundland and Labrador. This is what equity in actionlooks like: free, discreet access to essential health and harm reduction supplies, without fear, stigma, judgment, or barriers.
“Our Healthbox meets people where they are and puts compassion at the centre of care, helping to build healthier, more inclusive communities.”
The PDIFC Healthbox is one of two Newfoundland Healthbox units and one of eight in the Atlantic Provinces supported by Staples Canada, through their Even the Odds partnership with MAP.
There are now 24 Our Healthboxes across Canada, including recent launches in Alberta and the Northwest Territories.
These smart vending machines combine accessibility with real-time data analytics, tracking usage, ensuring supplies, and providing insights into community health trends for rapid, evidence-informed public health responses. To date, Our Healthboxes have reached more than 16,500people, distributing 1,800 HIV self-test kits, 4,100+ naloxone kits, 7,500+sexual health items, and more than 38,100 health and wellness supplies.
For more information about Our Healthbox, to track its progress, or to find a location near you, please visit www.ourhealthbox.ca.
About REACH Nexus at MAP Centre for Urban Health Solutions
REACH Nexus is a national research group focused on addressing HIV, Hepatitis C, and other sexually transmitted and blood-borne infections (STBBIs) in Canada. Based at the MAP Centre for Urban Health Solutions at St. Michael’s Hospital in Toronto, REACH works to reach the undiagnosed, expand testing options, connect people to care, improve access toprevention (PrEP and PEP), and reduce stigma.
About MAP Centre for Urban Health Solutions
MAP is Canada’s largest research centre focused on health equity and the social determinants of health. Internationally recognized for groundbreaking science and innovation, MAP develops and implements real-world, evidence-driven program and policy solutions that disrupt cycles of socio economic exclusion and poor health. For more than 25 years, MAP has partnered with communities and policy makers across the country to take on complex issues such as homelessness, intimate partner violence, inequitable access to healthcare and the prevention of opioid-related harms. MAP is based at St. Michael’s Hospital (Unity Health Toronto). Learn more at maphealth.ca.
REACH Nexus Contact Andrew Russell
Senior Communications Specialist
REACH Nexus – MAP Centre for Urban Health Solutions
andrew.russell@unityhealth.to
416-268-7642
How Ontarians’ chances of seeing a family doctor stack up against the rest of Canada
MAP scientist Dr. Tara Kiran spoke with the Toronto Star about OurCare’s latest report showing provincial variation in primary care access in Canada.
“It’s pretty clear we don’t have a national primary care system,” said Dr. Kiran, OurCare’s national lead and family physician at St. Michael’s Hospital in Toronto. “What we have are 13-plus different health and primary care systems, each getting different results.
Family doctor study finds disparities in primary care across Canada
MAP scientist and family doctor Dr. Tara Kiran spoke to The Globe and Mail about the latest survey conducted by OurCare research initiative. The latest results from the OurCare survey, show that just over 88 per cent of respondents in Ontario and Manitoba have a regular doctor, nurse practitioner (NP), or primary care clinic – the best results of any jurisdiction.
Fat signing bonuses, and concierge service, for family doctors
MAP Scientist Dr. Tara Kiran spoke to the New York Times for a story on Canada’s primary care system and efforts being taken to attract more family doctors, particularly in rural areas.
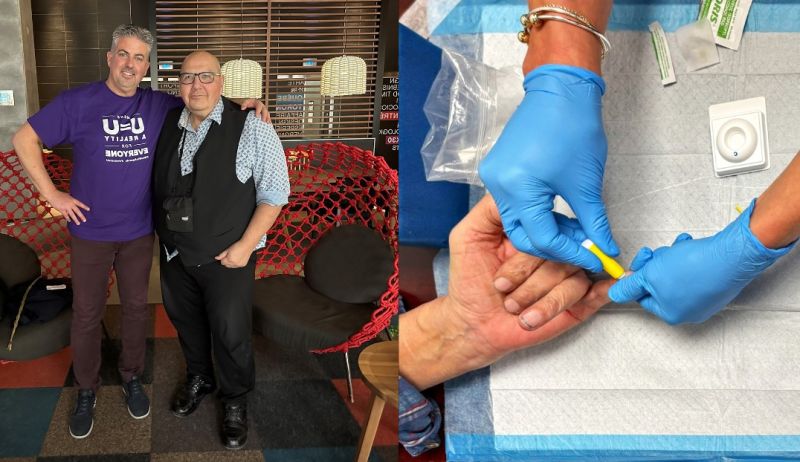
MAP co-led initiative reaches 2,000+ people in effort to curb rising HIV/Syphilis rates
Pictured above: Dr. Sean B. Rourke (left), a scientist with St. Michael’s MAP Centre for Urban Health Solutions, and Two Spirit Elder Albert McLeod attend a meeting for the Ayaangwaamiziwin Centre in April 2024. (right) a test for HIV/syphilis is performed as part of a community testing event.
Nearly one year after launching, more than 2,000 people have been enrolled in the Ayaangwaamiziwin Centre—a groundbreaking public health intervention tackling the soaring rates of HIV and syphilis across the Prairies and northern Territories.
Community and mobile testing across Saskatchewan, Alberta, and more recently Manitoba has identified +150 cases of syphilis and over 60 cases of HIV. People who tested positive received immediate treatment or were connected to culturally safe care and further preventative treatment.
Launched in March 2025, the Ayaangwaamiziwin Centre is a historic initiative, co-led with Indigenous communities designed to test, treat, and connect more than 11,500 people to trauma-informed, culturally grounded care. Working with community partners, including frontline health and harm reduction agencies, the Centre is currently operating at locations in the Prairies, with additional sites set to launch soon in Yukon, the Northwest Territories (N.W.T.), and Nunavut. Named after an Ojibwe word meaning “carefulness and preparedness,” the initiative is co-led by Dr. Sean B. Rourke, Director of REACH Nexus at the MAP Centre for Urban Health Solutions at St. Michael’s Hospital in Toronto.
“People are engaged and fascinated by this project. They love that they will be able to receive their results right then and there, at the same appointment rather than waiting days to receive results,” said Kristine Cockwill, an outreach worker with the Northreach Society, a harm reduction agency in Grand Prairie Alberta.
The Centre is aimed at helping people from Indigenous or remote communities who are often underserved by traditional healthcare systems. The model meets people where they are—whether in remote northern First Nations, urban shelters, or street encampments.
“Many people in these communities do not have a phone or any means of communication, making relaying positive cases back to the client challenging,” Cockwill said. “Rapid testing allows us to treat a positive syphilis case while the client is there and present for testing.”
A public health emergency
The Centre’s work comes at a critical moment. From 2020-2023, Canada has seen a roughly 85 per cent increase in new HIV diagnoses. In Saskatchewan and Manitoba, rates are three times the national average.
Each new HIV case carries an estimated $1.44 million in lifetime healthcare costs—totaling $2.1 billion for new cases in 2021 alone, an 11 per cent rise from a decade earlier (University of Alberta Institute for Health Economics).
Syphilis rates are also climbing at an alarming pace, nearly doubling between 2018 and 2023, from 6,371 to 12,135 cases.
Most devastating is the rise in congenital syphilis—passed from mother to baby during pregnancy. Once nearly eradicated in Canada, cases have surged by nearly 600 per cent, resulting in miscarriages, stillbirths, and infant deaths.
“The rise in congenital syphilis is a public health crisis—entirely preventable and entirely solvable,” said Dr. Rourke. “No baby in Canada should be born with this infection. With the right tools, testing, and care in the hands of those who need it most, we can end this.”
A coordinated national response
These numbers are more than statistics, they are a call to action.
The Centre is a bold, united response to the twin public health crises of syphilis and HIV with over 25 partners including:
- Public Health North Zone, Alberta Health Services in High Level, Alberta
- StreetWorks and Radius Community Health and Healing in Edmonton, Alberta
- Northreach Society in Grande Prairie, Alberta
- Wellness Wheel Medical Clinic and All Nations Hope Network in Regina, Saskatchewan
- Northern Inter-Tribal Health Authority in Prince Albert and northern Saskatchewan
- Ka Ni Kanichihk and Siloam Mission in Winnipeg, Manitoba
- One Yukon Coalition and Kwanlin Dün First Nation in Whitehorse, Yukon
- Chief Public Health Officers in Northwest Territories and Nunavut
These partnerships follow a “Two-Eyed Seeing” approach—blending Indigenous and Western knowledge systems.
“HIV and syphilis aren’t just statistics—they are public health emergencies tearing through communities,” said Dr. Rourke. “Every test, every diagnosis, every person we connect to care brings us closer to ending this crisis. We must act boldly, urgently, and together.”
The Centre is also preparing to deploy GeneXpert machines in clinics and mobile units to speed up diagnoses and provide rapid (even that day) treatment and referrals immediately. These machines can provide confirmatory testing in just under an hour and are a vital tool in remote communities where access to traditional labs is limited. It provides fast, accurate diagnoses on the spot, helping to connect people to treatment and culturally safe care.
A crisis decades in the making
The surge in sexually transmitted and blood-borne infections (STBBIs) in Indigenous communities is rooted in decades of systemic neglect, shaped by colonization, residential schools, intergenerational trauma, and ongoing structural racism.
“Indigenous-led, trauma-informed, and culturally safe care is essential to reducing STBBIs in First Nations, Inuit, and Métis communities,” said Dr. Tom Wong, Chief Medical Officer of Public Health at ISC.
“Everyone in Canada has the right to access health services and to thrive. But for many, that isn’t happening.”
Overcrowded housing, food insecurity, stigma, and discrimination all contribute to persistent health disparities and hinder care.
A human-centered approach
At its core, the Ayaangwaamiziwin Centre is about people, many of whom have been let down by existing systems.
Kristine Cockwill shared how she is able to reach individuals lost to follow-up—people who tested positive but never received care due to homelessness or legal issues.
“We identified a positive syphilis case at a community testing event using this point-of-care device and were able to treat the client immediately,” Cockwill said. “This was someone who likely wouldn’t have made it into an office and would have been very difficult to reach again. Being able to provide care on the spot was incredibly impactful.”
Building a new model of care
In March 2024, over 100 stakeholders—Indigenous leaders, Elders, health workers, and people with lived experience—gathered in Winnipeg to co-create community-driven solutions. Elder Albert McLeod introduced the group to the word Ayaangwaamiziwin, shared by Ojibwe Language Specialist Roger Roulette. The concept, “carefulness and preparedness, “now guides the entire initiative.
With deep partnerships, knowledge sharing, and a non-judgmental approach, the Centre shows what public health can look like when rooted in culture, dignity, safety and equity.
Over the next 3 years, the Centre will continue to expand, partnering with more frontline agencies and individuals with lived experience to reach those left behind by conventional healthcare.
“The Ayaangwaamiziwin Centre is a powerful shift in how we reach and honour Indigenous peoples and all those impacted by HIV, STBBIs, and systemic barriers,” said Albert McLeod.
“For too long, people have faced trauma, racism, and neglect in the health system. This Centre offers a new path—one rooted in dignity, healing, and self-determination. It’s about restoring trust, creating choice, and giving people the power to reclaim their health, their voice, and their future.”
By Andrew Russell
Opinion: Here’s one thing Mark Carney could do that would improve the welfare of more Canadians than any pipeline or mine
Dr. Nav Persaud, MAP scientist and Chair of the National Pharmacare Committee of Experts, wrote this op-ed for the Toronto Star framing national pharmacare as a necessary nation-building project.
Ontarians without a family doctor at higher risk of death, study finds
Dr. Tara Kiran, family physician and MAP scientist, spoke to Global News about a study that suggests Ontarians without a family doctor are at higher risk of death.
“You end up going for a lot of your care to walk-in clinics or emergency departments, and those settings are actually designed to just deal with an immediate issue,” Dr. Kiran said. “They don’t provide ongoing follow-up, and it’s not really their job to manage chronic conditions over time.”
Animal tranquilizer being mixed with fentanyl in Toronto’s illicit drug supply, experts warn
Hayley Thompson of Ontario’s Drug Checking Community, spoke to the CBC about powerful drugs used primarily by veterinarians to sedate animals increasingly showing up in Toronto’s unregulated drug supply.
Thunder Bay advocates push for emergency declaration over homelessness
MAP director and scientist Dr. Stephen Hwang, spoke to CBC News in Thunder Bay for a story about a possible state of emergency over homelessness in the community. Housing advocates and Indigenous leaders in Thunder Bay, Ont., have been calling on the city to declare a state of emergency over homelessness, while city staff are pushing for a humanitarian crisis to be declared, instead.