In 2016, we were successful in advocating for new municipal policy in Toronto that would open cold weather drop-ins earlier in the season, and allow them to remain open continuously over the coldest winter months. Our 2019 and 2023 studies prompted the City of Toronto to increase temperature thresholds for activating warming centres from -15C to -5C. An evidence-based brief summarizing the research remains one of the most-visited pages on the MAP website.
Category: MAP history
Research impact: Canada expands drug strategy to prevent more overdoses, provide additional services
Health Canada’s Substance Use and Addictions Program (SUAP) announced more than $21 million in federal funding for projects including the expansion of MAP’s multisite Drug Checking Service (a Canadian first) and our groundbreaking DoseCheck technology. This support will expand the life-saving services, promote our provincial monitoring of the unregulated drug supply, and directly contribute to better outcomes for people who use drugs.
Research impact: A roadmap for equitable Mpox vaccination
We were among the first to sound the alarm re: the equity implications of Mpox public health responses and related stigma, and the importance of global vaccine equity. We worked quickly to launch and complete a Mpox vaccine modelling study that provided a roadmap for vaccination.
Research impact: Canada approves first HIV self-tests in long-awaited move to reduce screening barriers
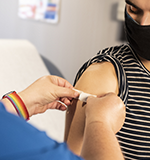
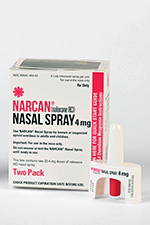
MAP research was instrumental in winning Health Canada’s landmark approval of the first HIV self-test in Canada: a one-minute, finger-prick blood test that can be purchased online and completed at home. Working together with community organizations, the health sector, and funders including Even the Odds, we are now distributing 50,000 HIV free self-testing kits across Canada through innovative mobile apps that support testing and connections to care, and “smart” vending machines that dispense HIV self-tests as well as free naloxone kits, harm reduction supplies and health information.
Research impact: COVID hits, MAP mobilizes to respond
When the pandemic struck, MAP scientists moved quickly to direct our expertise where it was most needed. MAP created COVID-19 data models to help front-line organizations predict spread in their local, client populations, led COVID-19 clinical trials, and worked to build a better health and social system. We provided expert opinion and informed public health responses in real time. MAP’s research showed that lower-income Toronto neighbourhoods were disproportionately impacted by COVID-19, which led to public policy that prioritized vaccinations for these hotspots. As Canada shifted focus to pandemic recovery, MAP launched a task force to identify the interventions and policy changes most likely to address COVID-19-related inequities in a post-pandemic world.
Research impact: Expert panel calls for $15B universal pharmacare
An advisory council set up by the Liberals proposed a national project to implement a universal public program for prescription drugs. Our first-of-its-kind research was endorsed and cited in the report as as a key resource and starting point for major pharmaceutical policy reform in Canada. In the years that followed, we continued to advance the pharmacare debate in Canada by proving that if everyone in Canada could access essential medications free of charge, it would not only improve the country’s health overall, but would save the health-care system billions of dollars.
Research impact: Province distributes naloxone to all inmates
Our research advanced advocacy leading to the Ontario Ministry of Health and Long-term Care’s life-saving decision to start distributing naloxone to inmates just prior to their release. Our studies showed that 10% of overdoses in Ontario were associated with release from incarceration, and that the highest-risk period was the first few days to two weeks after release – before most people can see a healthcare provider.
Research impact: National expansion of supervised injection facilities
Our research exploring the value and feasibility of supervised injection facilities was fundamental to establishing the evidence base for these services in Canada. Public health officials, community groups, and elected officials used our research to support applications to the federal government that resulted in the introduction of supervised injection facilities in Toronto. The Toronto Board of Health relied on these findings to appeal to the Federal Government to relax criminal restrictions on supervised injection.
Research impact: Embedding “Housing First” in Canadian policy
We led the Toronto arm of the Mental Health Commission of Canada At Home/Chez Soi study (2009-13), the largest randomized controlled trial in history to evaluate solutions to address homelessness. Our success testing the “Housing First” approach influenced the province of Ontario to set a goal to end chronic homelessness within the next ten years. Citing our evidence, the Ontario Ministry of Health and Long-Term Care also committed to invest $4M long-term funding to sustain housing and support to At Home participants in Toronto, and the federal government committed resources to scale up Housing First interventions across the country.
Research impact: Impossible to ignore: Homelessness and mortality
We were the first to quantify the profound impact that homelessness can have on a person’s life expectancy, proving that homeless men are eight times as likely to die as men in the general population. A large follow-up study, looking at 11 years of national data, found that among those who were homeless or marginally housed across Canada, the probability of survival to age 75 was only 32%. These stark findings were used to advance advocacy and policy arguments across Canada.